
How accurate are home tests? What men over 40 should know
Share
You’ve probably seen the marketing: “99% accurate,” “lab-quality results,” “trusted by thousands.” It sounds reassuring. But here’s the thing — not all home health tests are created equal, and accuracy isn’t just about the technology inside the box. For men over 40 managing real risks around STIs, fertility, and prostate health, understanding what those accuracy claims actually mean could be the difference between catching something early and missing it entirely. This article breaks down the facts so you can test smarter, not just faster.
Table of Contents
- Understanding home test accuracy: What does it really mean?
- How accurate are at-home STI tests for men over 40?
- Fertility and prostate cancer marker tests: Breakthrough or beware?
- How to get the most reliable results from home health tests
- Why the best home tests still require real-world caution
- Trusted home testing solutions for men over 40
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Accuracy varies widely | Home test reliability depends on the test type, user actions, and the health marker measured. |
| STI tests can be dependable | Lab-analyzed STI home tests for chlamydia and gonorrhea are accurate if instructions are followed exactly. |
| Cancer marker test caution | Rapid at-home PSA tests may give inaccurate prostate cancer results and should not replace professional screening. |
| Careful use boosts results | Following instructions and proper timing is critical to minimize false positives and negatives. |
| Confirm with professionals | Any worrying findings from home tests should always be discussed with a healthcare provider. |
Understanding home test accuracy: What does it really mean?
Let’s clarify what “accuracy” means so you can navigate misleading claims.
When a brand says their test is “99% accurate,” that number rarely tells the full story. Real accuracy in medical testing breaks down into several specific concepts, and each one matters differently depending on what you’re testing for.
Here are the key terms you need to know:
| Term | What it means | Why it matters |
|---|---|---|
| Sensitivity | How well a test detects a condition when it’s present | Low sensitivity means more false negatives — you might miss a real problem |
| Specificity | How well a test rules out a condition when it’s absent | Low specificity means more false positives — unnecessary worry or follow-up |
| False positive | Test says positive but you don’t actually have the condition | Can cause serious anxiety or unnecessary treatment |
| False negative | Test says negative but you actually do have the condition | Potentially dangerous — you walk away thinking you’re clear when you’re not |
| Overall accuracy | General percentage of correct results | Often used in marketing but doesn’t account for sensitivity or specificity separately |
Understanding what makes a test accurate goes beyond reading the box. A test might be highly specific but less sensitive, meaning it’s good at ruling something out but less reliable at catching it early.
There’s also a key distinction between lab-analyzed home tests (where you collect a sample and mail it off) and rapid self-read tests (where you read the result yourself at home in 15 minutes). Lab-analyzed tests generally offer more precision because trained equipment interprets the result. Rapid tests depend more heavily on your technique and how you read the result.
“Manufacturers commonly claim very high accuracy, but real-world issues such as sampling and instructions may limit this.”
That quote from a BMJ review of self-tests gets to the heart of it. The test might be accurate in a lab setting. Whether it stays accurate in your bathroom at 7am on a Tuesday is a different question entirely.
How accurate are at-home STI tests for men over 40?
Now that we’ve explained the fundamentals, let’s see how STI test accuracy plays out for men in your demographic.
The good news: home STI testing has come a long way. For chlamydia and gonorrhea specifically, at-home STI testing can be highly accurate when performed correctly — particularly when paired with lab analysis rather than a rapid read format. Studies consistently show sensitivities above 90% for these two infections when the sample is collected properly.

The challenge is that “collected properly” is doing a lot of heavy lifting in that sentence.
Here’s how accuracy compares across different approaches:
| Test type | Accuracy level | Coverage | Usability |
|---|---|---|---|
| Lab-based home test | High (90%+) | Chlamydia, gonorrhea, HIV, syphilis | Requires correct sample and mailing |
| Rapid home test (self-read) | Moderate to high | Usually 1-4 infections | Easiest to use but user-read errors possible |
| Clinic-based test | Very high | Broad panel | Requires appointment and travel |
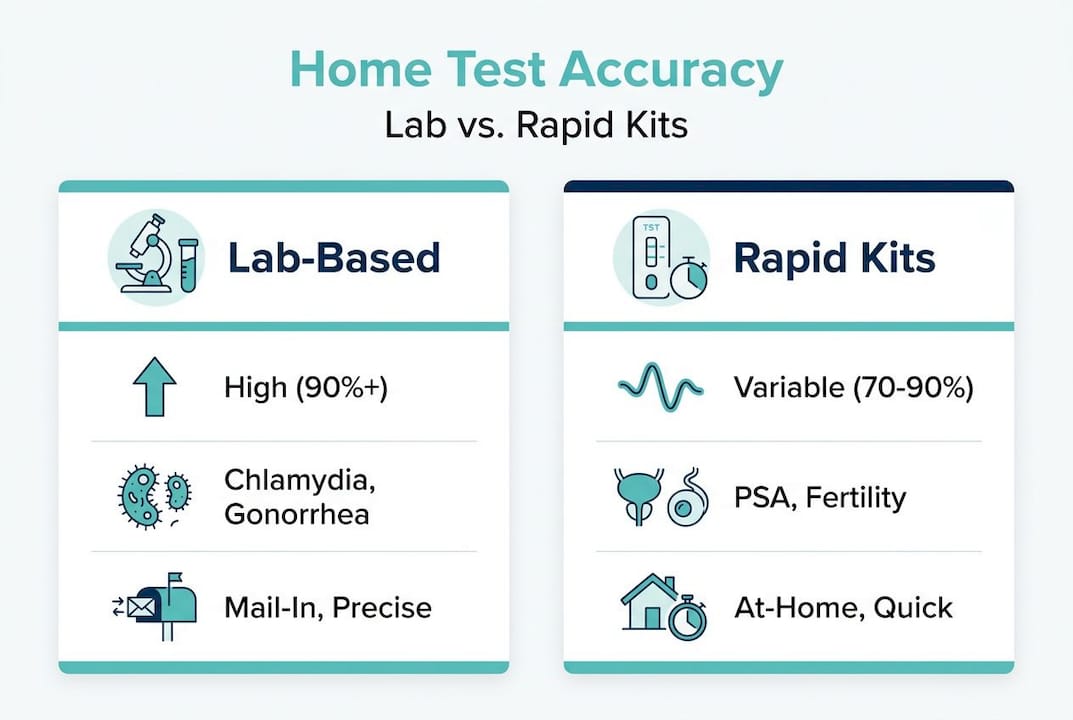
For men over 40, STI test accuracy is especially worth scrutinizing. Many men in this age group haven’t been tested in years, have new partners after separation or divorce, or simply assume STI risk decreases with age. It doesn’t. Chlamydia, gonorrhea, and syphilis rates are all rising in men over 40 across Europe and the UK.
Common reasons for false negatives in at-home STI tests:
- Testing too early after exposure (before the infection is detectable — known as the “window period”)
- Inadequate sample volume, for example not enough urine or a poorly swabbed area
- Mixing up swab types or using the wrong collection site
- Storing or posting the sample incorrectly
- Reading the result outside the recommended time window
Here’s a step-by-step approach for the most reliable results:
- Check the window period. Each STI has a different window period — the time after exposure during which the infection won’t yet show up. For HIV, that can be up to 45 days depending on the test type.
- Read the instructions first. All of them. Before you open anything.
- Use the right sample. Urine? Swab? Blood? Know which one applies to each infection in the panel.
- Time it correctly. Some tests require first-morning urine. Others require a specific volume collected mid-stream.
- Send promptly. If it’s a lab-based kit, don’t leave your sample sitting around. Temperature and time affect viability.
- Follow up if anything seems off. Unusual symptoms plus a negative result still warrants a professional check.
Pro Tip: If you’ve had unprotected sex with a new partner, don’t test immediately. Wait for the appropriate window period to pass, then test. An early negative result can create false confidence.
The benefits of home STI tests are real — no queues, no awkward waiting rooms, results you can act on quickly. But those benefits only play out if your technique is solid and your timing is right. Check safe STI self-testing tips before you start to make sure you’ve covered every base.
Fertility and prostate cancer marker tests: Breakthrough or beware?
STIs are only one piece of the health puzzle. Let’s address other tests that matter for men over 40 — fertility and cancer markers.
This is where things get more complicated, and where the gap between marketing claims and real-world performance is potentially most significant.
PSA testing and the prostate cancer question
PSA (prostate-specific antigen) is a protein produced by the prostate. Elevated levels can indicate prostate cancer, but also benign enlargement or infection. At-home PSA tests measure your PSA level from a finger-prick blood sample. Sounds simple. But a BBC investigation into rapid at-home PSA tests found them to be unreliable, with some kits producing inconsistent results and others missing known PSA elevations entirely.
In that investigation, only 1 of 5 PSA kits correctly flagged a false positive scenario. The others either gave no result or missed the elevation. That’s a significant real-world gap from the 98%+ accuracy figures you’ll see on packaging.
The broader issue with cancer marker testing is also well-documented. According to a PMC review on early cancer detection, early cancer detection tests including liquid biopsy approaches face real sensitivity and specificity limits. False positives can cause significant psychological distress and unnecessary procedures. False negatives can give you a false sense of security at exactly the wrong time.
Major pitfalls of home cancer and fertility marker tests:
- PSA levels fluctuate naturally. Exercise, recent ejaculation, and infection can temporarily raise PSA. A single reading without context is hard to interpret accurately.
- Fertility hormone readings require baseline comparisons. A single testosterone or FSH reading means little without knowing what’s normal for you.
- User technique affects blood sample quality. A poorly collected finger-prick sample can be too small, hemolyzed (broken-down blood cells), or contaminated.
- Rapid read tests are harder to interpret precisely. A faint line on a lateral flow test looks different to different eyes.
- No home test includes clinical consultation. Context, symptoms, and medical history matter enormously for interpreting cancer and fertility markers.
⚠️ Statistic to note: In BBC testing, multiple rapid PSA home kits failed to accurately reflect known PSA elevations. One in five gave a false positive. Others returned no usable result. This isn’t a rare outlier — it’s a documented pattern.
Pro Tip: If a home cancer marker test returns a concerning or unexpected result, don’t panic and don’t dismiss it. Book a follow-up with your GP or a private clinic for a confirmed lab-based test before drawing any conclusions.
The nuance around understanding cancer marker test risks is critical here. Home tests for PSA and fertility markers are useful screening tools when used correctly and interpreted with context. They are not standalone diagnostic instruments.
How to get the most reliable results from home health tests
With risks and opportunities clear, here’s how to make home testing work for you and your long-term health.
Whether you’re testing for an STI, checking your PSA level, or screening for fertility markers, the same core principles apply. The BMJ makes it clear: real-world performance depends heavily on mechanics — sample collection, timing, and interpretation.
Here’s a practical step-by-step guide to getting the most out of any home test:
- Store your kit correctly. Check the packaging for temperature requirements. Many kits degrade if stored somewhere too warm, like a bathroom cabinet above a radiator.
- Read the full instructions before you open anything. Not just the quick-start guide. The full leaflet. Every step.
- Check the expiry date. This sounds obvious, but it’s one of the most common mistakes people make.
- Prepare your sample according to exact specifications. Volume matters. Collection site matters. Timing matters (e.g., first-morning urine, no ejaculation 24 hours before a fertility test).
- Follow the timing instructions for reading results. Reading a rapid test at 10 minutes when the instructions say 15 can produce a misleading result.
- Photograph your result before discarding. If you need to discuss it with a professional later, a photo provides evidence.
- Note any factors that could affect accuracy. Recent illness, medication, sexual activity — mention these if you follow up with a clinician.
Review proper test technique tips specific to STI kits, and separately check reading at-home test results so you know exactly what you’re looking at when results appear.
“Even high-accuracy tests can be undermined by user technique or storage conditions. The test is only as reliable as the hands using it.”
When should you trust the result and when should you verify? As a rule:
- Negative result with no symptoms: Generally reassuring, especially with a high-sensitivity kit used at the right time.
- Positive result: Always confirm with a clinical lab before taking action or making decisions.
- Ambiguous or invalid result: Retest if a fresh kit is available, or go straight to a clinic.
- Negative result with ongoing symptoms: Don’t rely solely on the home test. See a professional.
Why the best home tests still require real-world caution
Here’s a perspective that often gets lost in the excitement around at-home health testing.
The numbers are impressive. Some kits genuinely perform at high accuracy in controlled conditions. And we’re big advocates for proactive home testing — getting men to check their health without the barrier of a waiting room is genuinely important.
But here’s the honest truth: accuracy in a lab and accuracy in real life are not the same thing. Every time a test leaves the controlled environment it was validated in, the risk of error increases. Not dramatically in most cases, but it’s real. And for men over 40, those small margins matter more because the stakes are higher. An undetected STI passed on. A missed PSA elevation. A fertility test result that sends you down the wrong path.
The balanced accuracy discussion we need to have isn’t about scaring people away from home testing. It’s about being honest that home tests are a powerful first step, not a final word. They are a tool in your health toolkit, not a replacement for clinical judgment.
The men who get the most value from home testing are the ones who follow the instructions precisely, understand the limitations, act on concerning results by seeking professional confirmation, and test regularly rather than treating it as a one-and-done event. That approach turns an 85% accurate rapid test into something genuinely meaningful. It’s not the kit alone — it’s how you use it.
Trusted home testing solutions for men over 40
If you’re ready to put this knowledge into practice, here are options designed for accuracy and peace of mind.
At Rapidtest, we’ve built our range specifically for people who want to take their health seriously without the hassle of clinics, queues, or awkward conversations. Our testing kits are evidence-backed, easy to use, and designed to give you reliable results in 15 minutes at home.
Whether you’re looking at at-home STI testing kits for peace of mind after a new partner, fertility testing kits to understand your reproductive health, or an at-home PSA test for prostate cancer screening — we have options that are straightforward, affordable, and designed to work. Every kit comes with clear instructions so you can test with confidence, not guesswork.
Frequently asked questions
Are home tests for STIs as accurate as those from a clinic?
For chlamydia and gonorrhea, lab-based home tests can be highly accurate when performed correctly, but user error and poor sample collection can reduce reliability compared to clinic testing.
How do I know if a home PSA test for prostate cancer is trustworthy?
Most rapid at-home PSA tests are less reliable than laboratory tests, with a BBC investigation showing several kits failed or produced false results — always confirm a concerning reading with a clinical lab.
What are the biggest mistakes to avoid with home test kits?
Incorrect sample collection and not following instructions exactly are the most impactful errors, as real-world performance depends directly on how accurately each step is followed.
Do home tests give false positives or negatives?
Yes, all home tests carry some risk of both — particularly for early detection scenarios, where early cancer marker tests have a documented risk of false positives and negatives due to sensitivity and specificity limits.
When should I see a doctor after a home test?
Consult a healthcare provider whenever you receive a positive result, an ambiguous reading, or if symptoms persist regardless of what the home test shows.

